In the most recent budget negotiations, Republican congressional leaders and the Obama administration inked a deal that will raise overall spending by $80 billion over the next two years and increases the federal borrowing limit. Yet it also includes cuts in Medicare spending and provisions aimed at reducing premium increases for Medicare beneficiaries.
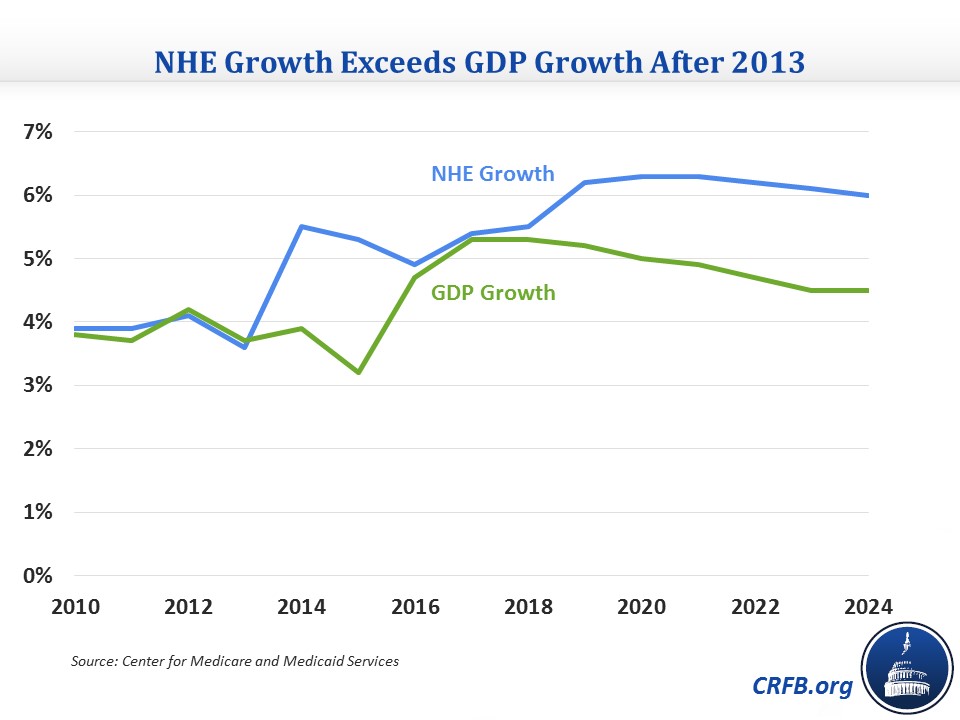
The legislation redefines the requirements for Hospital Outpatient Departments (HOPDs) and caps total payment for certain services at the physician rate. While the full economic impact has not yet been adequately defined, the Medicare Payment Advisory Commission (MedPAC) estimates that this would cut spending by $1.44 billion (2.7%) in one year, and will enable 30% of Medicare Part B beneficiaries to avoid a looming 52% spike in premiums. According to the Wall Street Journal, Medicare Part B premiums will only increase by approximately 15%. Both the American Hospital Association and the Association of American Medical Colleges have strongly opposed the legislation, citing inadequate provisions for the unique costs and regulatory requirements of HOPDs and a reduction in patient access to care.
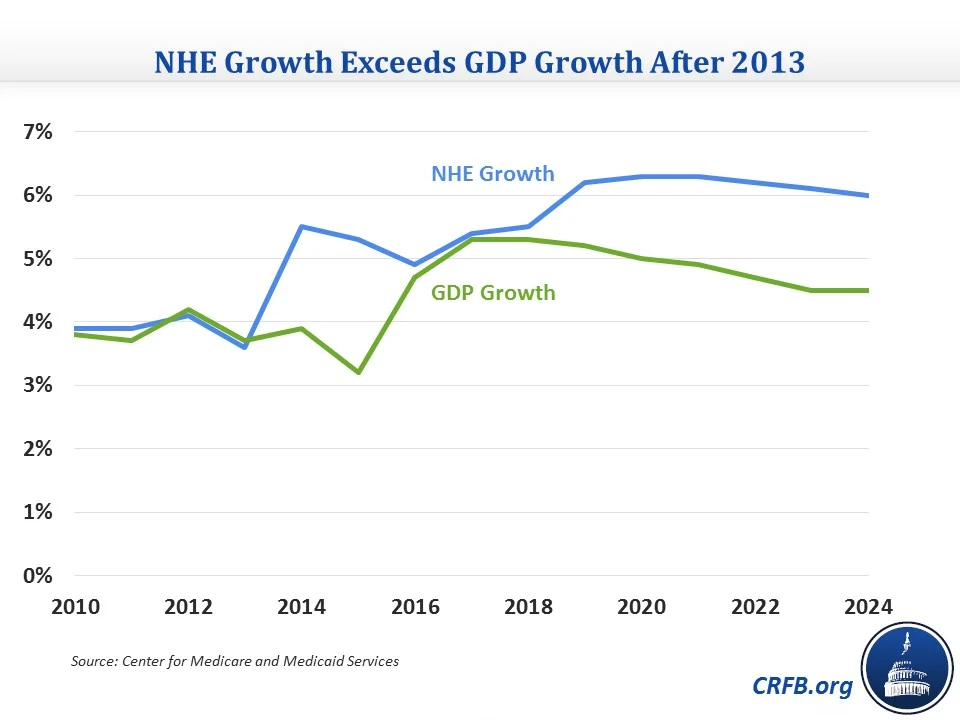 However, it does attempt to ease the transition for health systems, allowing existing provider-based outpatient departments to be grandfathered. It is the definition of “existing” that is concerning many systems currently. According to the bill, if the HOPD bills prior to the enactment of the law (prior to November 2, 2015), then it would be covered under the grandfather clause. Many systems accelerated plans for HOPD developments that were underway, and are now re-thinking projects that are still in the conceptual phase. Undeniably this legislation is having a major impact on physician alignment, clinical service distribution and on facilities and healthcare real estate strategy.
However, it does attempt to ease the transition for health systems, allowing existing provider-based outpatient departments to be grandfathered. It is the definition of “existing” that is concerning many systems currently. According to the bill, if the HOPD bills prior to the enactment of the law (prior to November 2, 2015), then it would be covered under the grandfather clause. Many systems accelerated plans for HOPD developments that were underway, and are now re-thinking projects that are still in the conceptual phase. Undeniably this legislation is having a major impact on physician alignment, clinical service distribution and on facilities and healthcare real estate strategy.
We at Array are working with many health systems that are exploring the strategic impact of this legislation, and in this next series of posts we will survey and report upon some of the more innovative approaches to minimizing the economic impact upon the system without sacrificing access and patient care.

